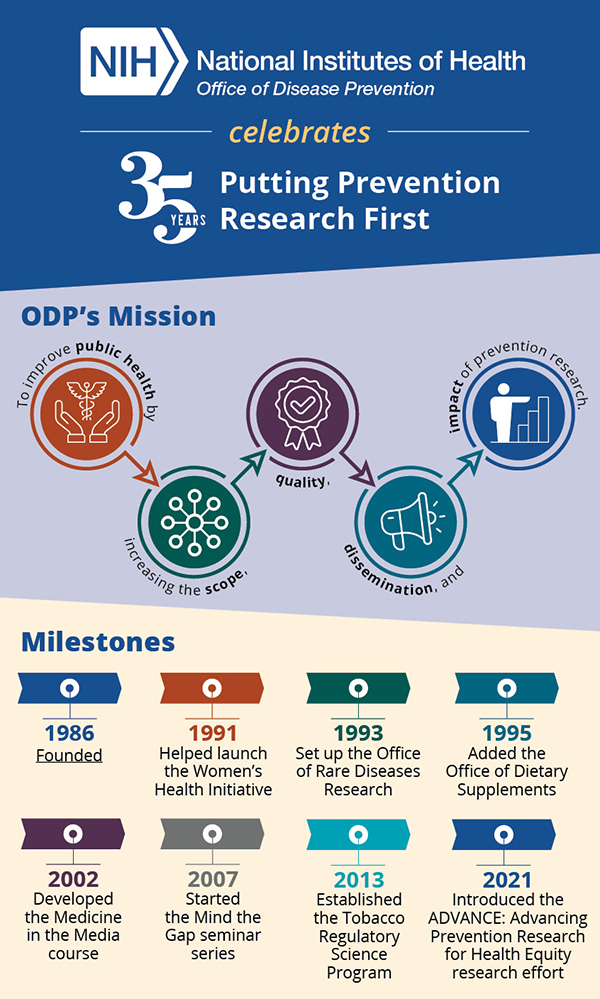
I’m honored to mark the 35th anniversary of the ODP. Our Office was founded in 1986 to promote and coordinate prevention research across the NIH and with other public and private partners. The field has changed dramatically since then. To get a sense of how much has been accomplished, ODP staff and I took some time to consider the past, present, and future of prevention research.
How has the field of prevention research evolved since 1986?
When the ODP was founded, prevention research was focused heavily on infectious diseases. For example, the goal to eliminate polio in the Americas was set in 1985 and several vaccines were first licensed in the 1980s, including a vaccine against Hepatitis B and the oral typhoid vaccine.
Over time, attention has shifted to preventing chronic disease. Three community-based heart disease prevention projects funded by the National Heart, Lung, and Blood Institute in the 1980s set the stage for the rapid growth of group- or cluster-randomized trials in prevention research. In the years that followed, we saw an increasing number of worksite-based trials to address risk factors for cardiovascular disease and cancer; school-based trials to address adolescent use of alcohol, tobacco, and other drugs; clinic-based trials for smoking cessation; and many more.
At the same time, rapid developments were made in the methods for those trials. Until about 10 years ago, prevention research relied on traditional methods for observational research and clinical trials. We have seen a shift to newer methods, such as pragmatic trials, in an effort to make prevention research less expensive and more easily implemented in practice.
Biomedical research has also begun to move away from its historical focus on white men. The Women’s Health Initiative, originally led by the ODP’s third director, Dr. William Harlan, was launched in 1991 as the first large-scale prevention trial focused exclusively on women. The NIH Office for Research on Women’s Health was created in 1993, and the NIH required inclusion of women in all research in 1994. Although inclusion of racial and ethnic minority groups in prevention research still lags behind that of white persons, the NIH is making concerted efforts through initiatives like UNITE to address health disparities and improve health equity research.
What are some ways that the ODP has helped advance the field over the last 35 years?
We encourage you to explore our History of the ODP timeline and our new infographic for a fuller look at our work over the years. Listed below are some highlights.
- The ODP became the home of the Consensus Development Program (CDP). Consensus conferences, which began in 1977, had a major influence on public health practice in areas like breast cancer screening, knee replacement surgery, and the use of prenatal steroids for prevention of premature birth.
- Since the ODP led the NIH scientific review of the first edition of the Guide to Clinical Preventive Services in 1989, we have been the NIH’s liaison office for the U.S. Preventive Services Task Force (USPSTF). Our partnership has led to increased attention to the evidence gaps identified by the USPSTF and to more NIH funding opportunity announcements targeting those gaps.
- The ODP has served as the NIH’s liaison office for the Department of Health and Human Services’ Healthy People initiative since the 1990s. The ODP contributes to the development of Healthy People objectives and helps recruit NIH staff to serve on Healthy People workgroups.
- When the CDP was retired in 2013, the ODP launched the Pathways to Prevention (P2P) workshop series. P2P workshops use an unbiased, evidence-based process to identify research gaps in a scientific area of broad public health importance and suggest ways to move the field forward. Workshops have highlighted research needs in fields like obesity prevention, the use of long-term opioid therapy for chronic pain, youth suicide prevention, and most recently, improving health outcomes in rural areas through provider-to-provider telehealth.
- The Tobacco Regulatory Science Program (TRSP) was established within the ODP in 2013 to coordinate and support research to inform the Food and Drug Administration’s (FDA) regulation of tobacco products, which remain the number one cause for death and disability in the United States.
- The ODP began to analyze the NIH prevention research portfolio in 2013. This effort provided the first thorough examination of how much of the NIH research portfolio is dedicated to prevention (20.7% of all NIH research projects in 2019) and how those projects are distributed across a wide variety of topics. It also helped us identify important gaps in the NIH prevention research portfolio.
How can we build on this progress?
Looking forward to our next 35 years, some major areas of focus for the ODP include:
- Working to achieve health equity in disease prevention. A critical part of reducing health disparities involves addressing the leading risk factors and causes of death and disability, many of which can be prevented, delayed, or caught and treated early. However, through our portfolio analysis work, we found the NIH has not supported much intervention research to address these risk factors in populations that experience health disparities in the United States. In response, the ODP is launching a long-term, NIH-wide effort called ADVANCE: Advancing Prevention Research for Health Equity.
- Reducing tobacco use. Equipped with the evidence generated by TRSP, the FDA is taking action to regulate electronic nicotine delivery systems, such as e-cigarettes and vape pens, that exploded in popularity over the last 10 years.
- Continued development and adoption of better research methods. The ODP is working hard to provide NIH staff and the extramural community with resources to better plan, design, conduct, and analyze rigorous research studies, including those using group-based interventions.
- Advancing research to inform preventive service recommendations. We will continue engaging our NIH colleagues to address evidence gaps identified by the USPSTF. Filling these gaps will allow the USPSTF to broaden its recommendations to cover additional populations and to address additional conditions that adversely affect the health of the nation.
While we have a great deal of work to do, we look forward to continuing to advance prevention research through developing and implementing evidence-based interventions to improve the health of our nation for all.
To stay up-to-date with ODP news and events, please follow us on Twitter and subscribe to our email updates.